is a condition where there is a misalignment of the eyes.
Strabismus or squint is a condition where there is a misalignment of the eyes. The types of strabismus vary among different age groups and present differently in different parts of the world. In Asia, exotropias or divergent squints are the most common type of strabismus, consisting of 65%-85% of total childhood strabismus. On the flip side, esotropias or convergent squints are 2-4 times more common in the West than exotropias.
It is important to distinguish a comitant from an incomitant squint. A comitant squint is one where the angle of the ocular deviation is similar in all directions of gaze, whereas an incomitant squint is one where there is a difference in the angle of the deviation in different directions of gaze.
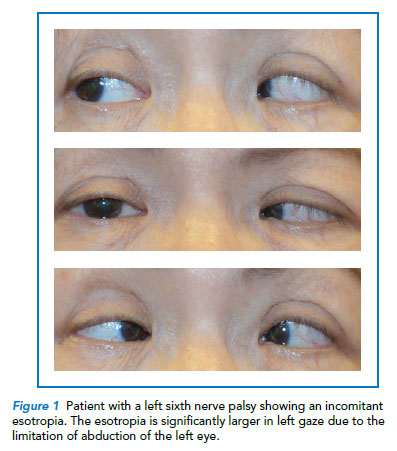
Comitant squints are characteristically found in patients with congenital or early-onset strabismus. On the other hand, incomitant squints are usually a result of a restrictive cause (a tight intraocular muscle in thyroid eye disease), or a paralytic cause (an acute sixth nerve palsy causing limitation in abduction of the lateral rectus muscle on the affected side). As a result, limitation of eye movement is usually present in such cases and is an important differentiating factor (Refer to Figure 1).
This article will focus mainly on comitant squints encountered in children, their features, and treatment and clinical assessment.
ESOTROPIA
Pseudoesotropia
In a survey performed at the Singapore National Eye Centre (SNEC) and KK Women’s and Children’s Hospital (KKH) from 2000-2002, pseudoesotropia was found to be the most commonly encountered ‘squint’ in our clinics. This is due to Asian babies having a flatter nose bridge and wider epicanthic folds, giving the false impression of a convergent squint (Refer to Figure 2).
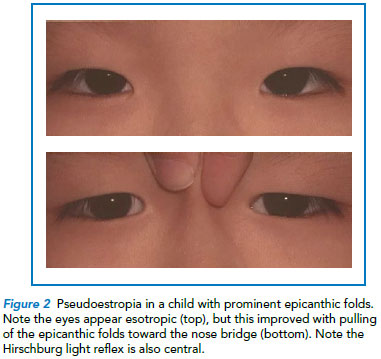
While reassuring parents that their child does not have a true squint, this does not mean they will not develop an actual strabismus later in life, and parents need to be advised to return if there is a change in the eye alignment.
Infantile Esotropia
Infantile esotropia is a constant, large angle esotropia (usually more than 30 prism diopters) that typically appears before the age of 6 months.
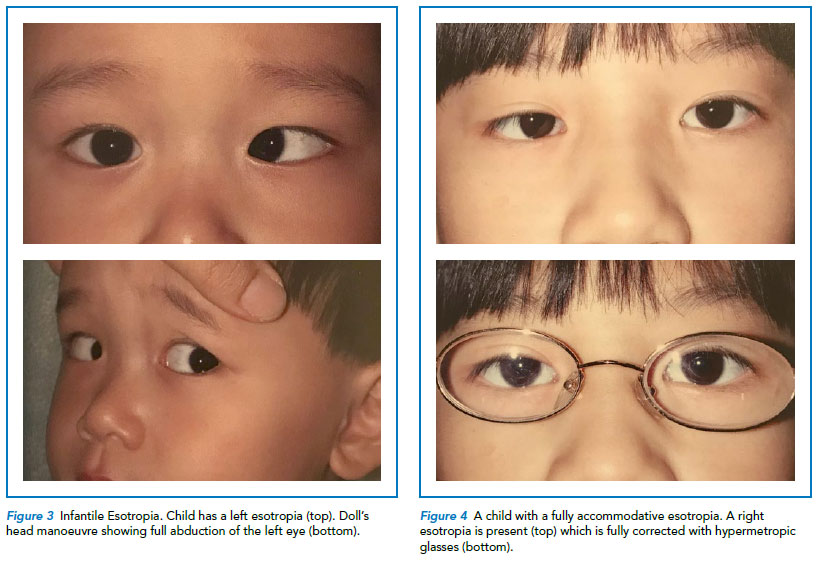
It is important to assess the ability of the eye to fully abduct, in order to differentiate it from a lateral rectus (sixth nerve) palsy that could be life-threatening. In children, where getting them to follow a target may be difficult, performing the doll’s eye manoeuvre can be useful (Refer to Figure 3).
Surgery is the treatment of choice in this condition, though the best time for it is still controversial.
However, the general consensus is that it should be performed before the age of 18 months to give the child a better chance of developing binocular function.
Accommodative Esotropia
This type of esotropia usually appears between the ages of 18-36 months, but can occur as early as 2 months and up to 6 years of age. It is related to excessive hypermetropia, resulting in overaction of the accommodative reflex.
Accommodative esotropia can be completely or partially corrected with glasses.
In a child with a fully accommodative esotropia, the convergent squint is eliminated completely with the use of glasses to correct the full amount of hyperopic refractive error (Refer to Figure 4). It is important that glasses are worn full-time.
In those with partially accommodative esotropia, glasses will only correct part of the squint and surgery will be required to correct the residual deviation.
Near vision involves both accommodation and convergence. In some cases of accommodative esotropia, the deviation at near is significantly larger than that at distance. This is due to a high Accommodative Convergence/Accommodation (AC/A) ratio, in which a unit of accommodation is accompanied by a disproportionately large amount of convergence.
Children with a high AC/A ratio have an esotropia which is larger angle at near, and require the use of executive bifocal glasses to help correct their near misalignment.
EXOTROPIA
Of the true squints that are seen in our clinics, intermittent exotropias are the most common and consist of approximately 60% of cases seen in our clinics.
Intermittent Exotropia
As its name suggests, this outward exodeviation tends to occur intermittently. At times, the child is able to control the exodeviation, and at other times is unable and breaks down into a manifest exotropia (Refer to Figure 5).
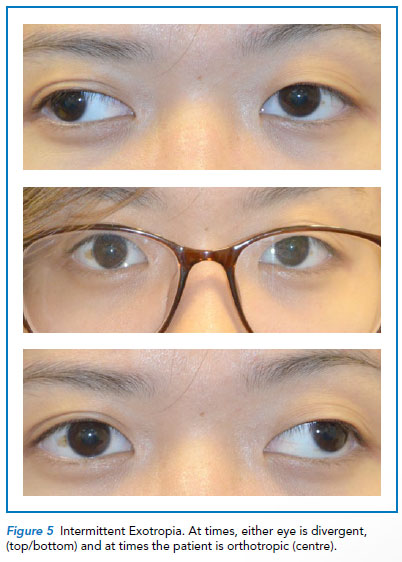
However, some patients may progress from exophoria to Intermittent Exotropia (IXT), and then to constant exotropia. The size of the exotropia can also change over time.
Patients with intermittent exotropia can present with varying degrees of control. If control is good, ocular alignment is often maintained and eyes do not dissociate or deviate easily. However, if control is poor, patients may frequently exhibit a manifest exotropia.
Intermittent exotropia can be broadly classified into 3 types:
1. Basic IXT: where the exotropia measures similarly at near and distance
2. Convergence insufficiency IXT: where the exotropia measures larger at near compared to distance
3. Divergence excess IXT: where the exotropia measures larger at distance compared to near (divergence excess)
The onset of IXT is usually in early childhood. It can be precipitated by illness, tiredness, and bright light or daydreaming.
Children may blink in order to regain binocular function or close 1 eye under bright light, the symptom that is sometimes first noticed by parents. Some children may also experience eyestrain or headaches as they try to maintain binocular fusion by accommodation and convergence.
TREATMENT
Treatment options for IXT include convergence or fusion exercises, patching, over-minus lenses and surgical correction. Generally, if control were good to moderate, non-surgical treatment would suffice.
The MyEyeGym application is an orthoptic eye exercise application developed by the Singapore National Eye Centre (SNEC) for people with an intermittent squint. It allows users to perform different types of fusional exercises using their handheld smart devices (Refer to Figure 6).
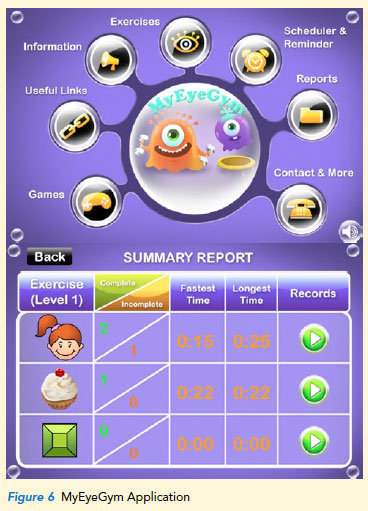
At the same time, there is also a progress and summary report with daily reminders that can motivate children to perform their exercises regularly. In general, these fusional exercises would be useful only in older children as a degree of understanding would be required.
Children who would benefit from surgery include those with poor or deteriorating fusion, increasing frequency of breakdown of their IXT, increasing size of the exodeviation or increasing symptoms of asthenopia. However, if possible, surgery should be performed when the child is older than 4 years of age to minimise problems encountered with overcorrection.
CLINICAL ASSESSMENT OF A CHILD WITH A SUSPECTED SQUINT
A thorough history is important. Important factors include:
- The age of onset
- The character of the squint: intermittent or constant
- Its evolution: more or less frequent, whether there is a fixation preference (especially important in younger children less than 8 years old where there is a risk of amblyopia)
- Any predisposing factors: trauma, illness etc.
- Any other associated symptoms: such as diplopia (that may suggest an acute onset or an incomitant cause), headache, nausea or vomiting (that may suggest more dangerous causes, such as raised intracranial pressure resulting in a false localising sign)
In younger children whose vision is not yet fully developed (those under 8 years old), a frequent or constant deviation of 1 eye can result in amblyopia-decreased visual acuity, as a result of monocular suppression of the deviating eye. Hence an accurate visual assessment is important.
In older children, visual acuity can be assessed using the Snellen visual acuity chart. For preverbal children, specialised visual acuity tests that work on the basis of preferential looking (Refer to Figure 7) are available in our clinics.

Vision in these younger children can also be grossly assessed
by the child’s fixation behaviour. The ability of a child to maintain
central steady fixation, and fix and follow a target with
their eyes can be assessed using a brightly coloured toy (or
your face!). Occlusion of either eye at a time may reveal a
preference for the use of 1 eye and a poorer visual acuity in
the other, if a child objects strongly to the occlusion of 1 eye.
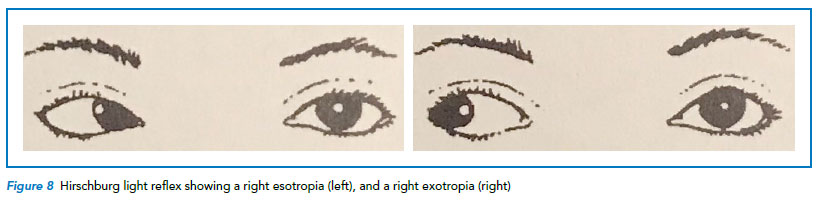
Observe the child for any gross ocular misalignment. A simple
Hirschberg (pupil light reflex) can reveal the presence of a
manifest squint (Refer to Figure 8). A cover uncover test can bring forth a latent squint (e.g. an intermittent exotropia with
control). Ocular motility should be tested, and both versions
and ductions assessed, to examine the range of eye movements
and any limitations present.
All children with a squint will require a complete ocular examination
to exclude any potential ocular causes of poor vision
resulting in a squint, for example, a unilateral congenital cataract
resulting in poor vision and hence, exodeviation of that
eye. Therefore, in all children with suspected strabismus, a
referral to an ophthalmologist should be made.
Dr Tay Su Ann is a Consultant at the Department of Paediatric Ophthalmology and
Adult Strabismus at the Singapore National Eye Centre (SNEC). Her areas of interest
are in childhood myopia and paediatric neuro-ophthalmology.
GPs can call for appointments through the GP Appointment Hotline
at 6322 9399 or more information.
REFERENCES:
1. Clinical Ophthalmology-An Asian Perspective. Saunders Elsevier 2005
2. Kornder LD et al. Detection of manifest strabismus in young children. A prospective study. Am J Ophthlamol 1973;8:244-51
3. Graham PA. Epidemiology of strabismus. Br J Ophthalmol 1974;58:224-31
4. Yu CB et al. Changing patterns of strabismus: a decade of experience in Hong Kong. Br J Ophthalmol 2002;86:854-6
5. Chia A, Quah BL, Seenyen L. Progression of intermittent exotropia amongst children in Singapore. AAPOS Meeting, Orlando, FL 2001.
Poster.
6. Pratt-Johnson JA et al. Early surgery in intermittent exotropia. Am J Ophthalmol 1977;84:689-94
